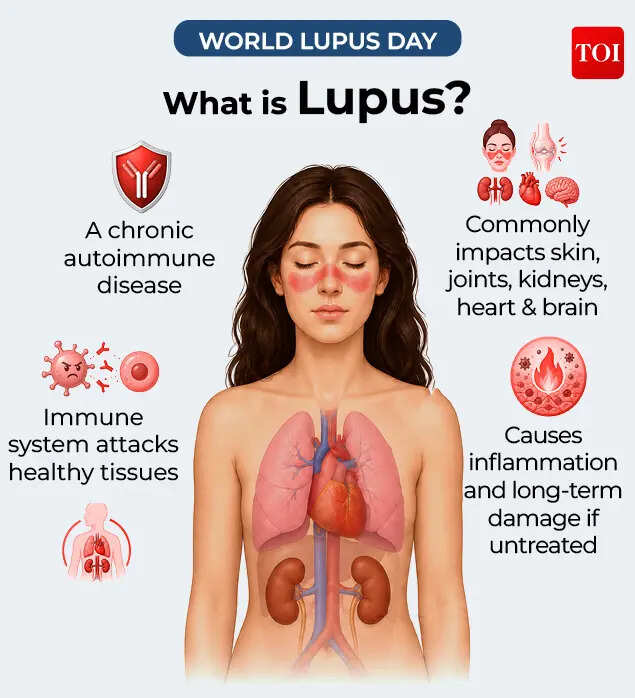
‘You’re probably just stressed.’ For many women living with lupus, that is often where the story begins. A young woman walks into a clinic complaining of fatigue, joint aches, hair fall, fever or persistent body pain.Instead of answers, she is told she is overworked, anxious, sleep-deprived, hormonal or simply exhausted from balancing work, family and daily life.Some are advised to take iron supplements for anaemia, others are treated for depression, thyroid disorders, viral infections or chronic fatigue. But the symptoms do not go away.Months and sometimes years can pass before doctors finally identify the real cause: lupus, a chronic autoimmune disease in which the body’s immune system mistakenly attacks its own healthy tissues and organs. By the time many women receive a diagnosis, the disease may already be affecting the kidneys, joints, skin, heart, lungs or even the brain.This World Lupus Day, let’s turn our attention to a condition often described as an ‘invisible illness’ because its impact is not always visible, but deeply life-altering.
.
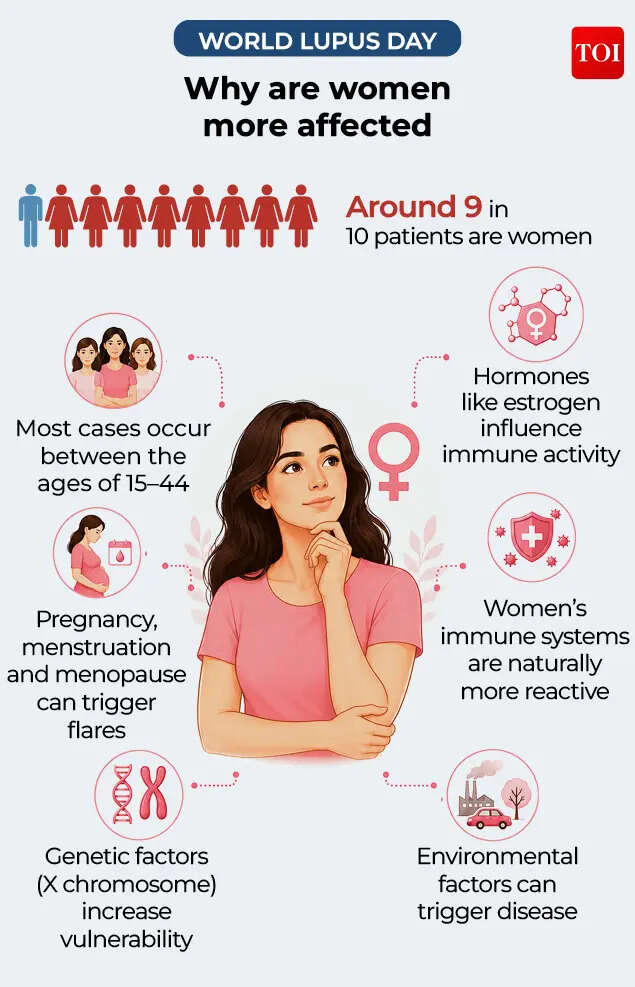
One of the biggest challenges with lupus is that its early signs are vague and unpredictable. Fatigue, joint pain, fever, hair loss, rashes and memory issues can occur for multiple reasons, making early detection difficult.The numbers, however, reveal a striking pattern. According to research at Cornell Medical University, around 9 out of 10 lupus patients are women, with most diagnoses occurring between the ages of 15 and 44.Researchers believe hormones, genetics, immune system differences and environmental triggers together make women significantly more vulnerable to the disease.Dr Geetika Jassal, medical spokesperson at Cryoviva Life Sciences, says lupus is far more than just a condition affecting the skin or joints and awareness remains one of the biggest gaps in early diagnosis.“Lupus affects women far more commonly than men, particularly during the reproductive years. According to CDC (Center for Disease Control and Prevention) nearly 9 out of 10 people diagnosed with lupus are women, and women aged between 15-44 years are at highest risk. This strong gender difference highlights the complex interaction between hormones, immunity, genetics, and inflammation in women’s health. Lupus is not just a skin or joint disease; it is a chronic autoimmune disorder that can affect multiple organs. This is why early awareness, timely diagnosis, and long-term monitoring are extremely important,” she said.
Lupus explained: When immune system turns against the body
Lupus is a chronic autoimmune disease, but to understand it simply, it helps first to understand what “autoimmune” means. Normally, the immune system acts like the body’s defence force, identifying and attacking harmful invaders such as viruses and bacteria. In lupus, however, this defence system becomes confused and starts targeting the body’s own healthy cells and tissues.Instead of protecting the body, the immune system begins attacking it from within. This can trigger inflammation, a process where the body becomes swollen, irritated and damaged as immune cells mistakenly attack healthy organs. Over time, this ongoing inflammation can affect different parts of the body and disrupt how they function.What makes lupus different from many other autoimmune diseases is that it is systemic in nature. While some autoimmune conditions primarily target one area like joints or the thyroid gland. Lupus can affect multiple organs at the same time. The skin, joints, kidneys, heart, lungs, blood vessels and even the brain may all be involved, which is why symptoms can feel scattered and unrelated at first.At a cellular level, lupus is linked to antinuclear antibodies (ANA), proteins that mistakenly target the nucleus of cells. These antibodies can form immune complexes that settle in tissues and trigger further inflammation and damage.Because of this wide-ranging impact, lupus does not follow a single predictable pattern. It can look different in every patient, which is one of the reasons it is so difficult to identify early and often gets confused with other conditions.
Why does lupus hit women harder than men?
Lupus shows a strong gender bias, with women forming the vast majority of cases. Researchers believe this is due to a combination of hormonal, genetic and environmental factors.
a) The estrogen connection
Women have higher estrogen levels, especially during reproductive years, the same period when lupus is most commonly diagnosed.Hormonal fluctuations during menstruation, pregnancy and menopause can influence immune activity and trigger flares in susceptible individuals.
.
b) The X chromosome theory
Another important factor lies in genetics. Women have two X chromosomes, while men have one X and one Y chromosome. Certain immune-related genes are located on the X chromosome and variations in how these genes are regulated may increase immune sensitivity in women.In simple terms, women’s immune systems tend to be more reactive. While this can offer stronger protection against infections, it can also increase the risk of the immune system turning against the body.
c) Genetics and environmental factors can trigger disease
Genetics alone does not cause lupus; it creates susceptibility. A family history of autoimmune disease can increase risk, but most people with lupus do not have a direct family link.Environmental factors often act as triggers that “activate” the disease in genetically prone individuals. These include sunlight exposure, viral infections, chronic stress, smoking, pollution, and certain chemical exposures. According to Associated Press, researchers also point to viruses like Epstein-Barr as possible contributors that may disrupt immune regulation and initiate disease processes in some cases.
Symptoms that women often ignore until lupus becomes serious
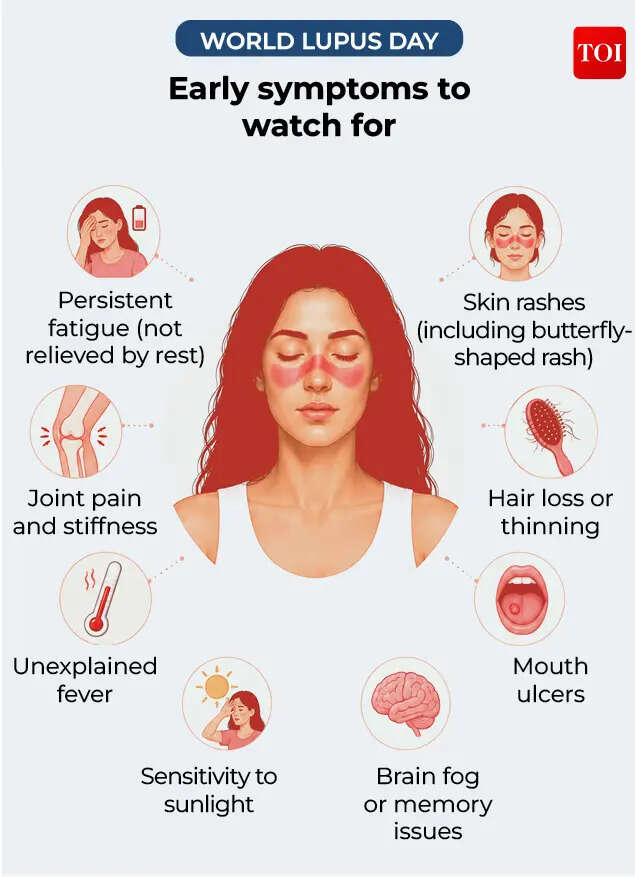
Lupus often begins with symptoms that are easy to dismiss.These include fatigue that does not improve with rest, joint pain, fever, hair loss, mouth ulcers, sun sensitivity, brain fog and butterfly-shaped facial rashes.Individually, they may seem minor. Together, they can signal ongoing autoimmune activity.
.
However, these symptoms are frequently mistaken for stress, burnout, thyroid issues, hormonal imbalance or viral infections.According to Dr Geetika Jassal, one of the biggest challenges is that lupus symptoms often resemble common health complaints.“The early symptoms of lupus are often mistaken for common conditions like tiredness, stress, vitamin deficiencies, viral infections, allergies or general body pains. Many women may experience persistent fatigue, pain or swelling joints, unexplained fever, hair loss, mouth ulcers, skin rashes, and sensitivity to light. One of the challenges with lupus is that these symptoms may appear intermittently and vary in intensity, which can delay diagnosis,” she said.
Why is lupus called an ‘invisible illness’?
Lupus is often called an invisible illness because patients may appear healthy while experiencing severe internal symptoms.Chronic fatigue, fluctuating pain and brain fog can make daily life difficult, even when no visible signs are present.Symptoms often come and go, which makes the condition harder to understand for others and sometimes even for patients themselves.This invisibility often leads to misunderstanding in workplaces and social settings, contributing to emotional strain and isolation.According to Dr Geetika Jassal, lupus is often misunderstood because many symptoms remain invisible to others.“Lupus is often referred to as an invisible illness since many of its symptoms are not always visible from the outside. A woman with lupus may appear healthy externally while silently struggling with severe fatigue, chronic pain, brain fog, inflammation, flare-ups, or even internal organ involvement. This can sometimes lead to misunderstanding at home, in workplace and within society, as others may not fully recognize the physical and emotional burden of the disease,” she said.
Why women of colour face a greater lupus burden
Lupus does not affect all women equally. According to research at New York University, it has consistently shown that women of colour, particularly Black, Hispanic, Asian and Indigenous women, face a higher risk of developing the disease, often at a younger age and with more severe outcomes.Studies indicate that Black women are up to three times more likely to develop lupus compared to white women. Similar patterns are seen among Hispanic and Asian women, who are also more likely to experience earlier onset of symptoms. The reasons behind this disparity are complex and interconnected. Genetics may play a role in increasing susceptibility, but they do not act alone. Differences in healthcare access, delayed diagnosis, socioeconomic barriers and uneven exposure to environmental stressors all contribute to how the disease is experienced and managed.
When lupus turns dangerous: The organs it can damage
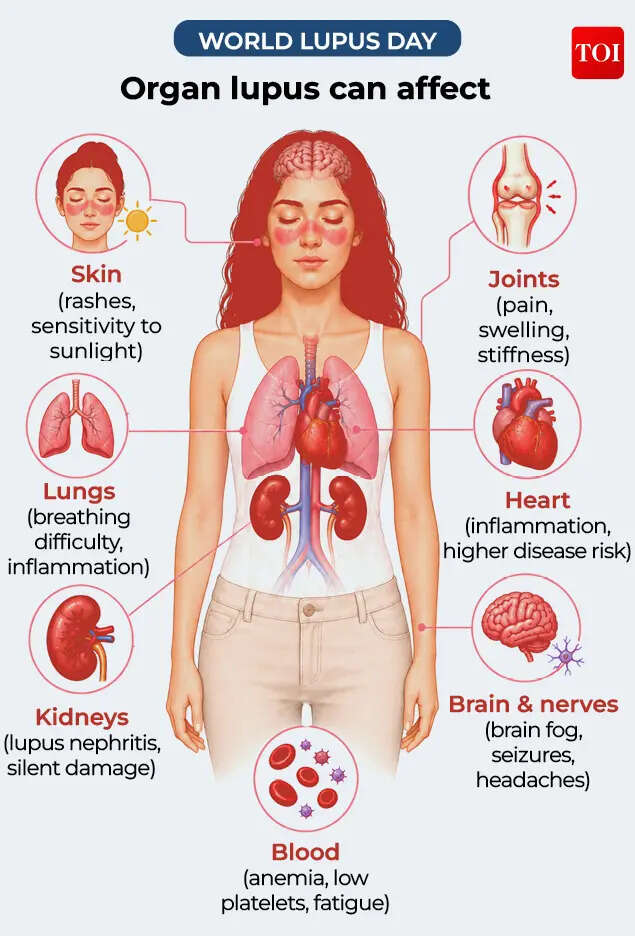
Lupus can quietly affect internal organs even when external symptoms appear mild.
.
- Heart: Increases risk of inflammation and early cardiovascular disease.
- Kidneys: Can cause lupus nephritis, often without early symptoms.
- Brain & nervous system: May lead to brain fog, seizures, headaches, stroke risk.
- Bones: Long-term inflammation and steroid use increase osteoporosis risk.
- Pregnancy: Raises risk of miscarriage, preterm birth and neonatal lupus; requires high-risk monitoring.
Why is lupus so difficult to diagnose
Lupus is widely known as one of the most challenging autoimmune diseases to diagnose, not because it is rare, but because it rarely presents straightforwardly or predictably. There is no single test that can confirm lupus on its own, which often makes the diagnostic process long and complex.One of the most commonly used screening tools is the ANA (antinuclear antibody) test. However, this test alone is not definitive. A positive ANA result can be seen in lupus, but it can also appear in other autoimmune conditions or even in healthy individuals, which can create confusion and lead to uncertainty in early evaluation.Another major challenge is that lupus symptoms overlap with many other conditions. Fatigue, joint pain, fever, skin rashes and hair loss can all be linked to thyroid disorders, viral infections, chronic fatigue syndrome or even stress-related conditions. As a result, many women consult several doctors over months or even years before receiving a clear diagnosis. In many cases, lupus is only identified after ruling out other possible conditions, a process known as “diagnosis by exclusion.”Because of its complexity, rheumatologists play a critical role in identifying lupus early. Their specialised understanding of autoimmune diseases helps connect seemingly unrelated symptoms into a single underlying condition, which is often missed in general evaluations.
Can the disease be cured?
Lupus is a lifelong condition and at present there is no permanent cure. However, with timely diagnosis, appropriate treatment and consistent care, the disease can often be managed effectively.Medical treatment is the cornerstone of lupus management. Commonly used medical treatments include hydroxychloroquine, corticosteroids, immunosuppressants and biologic therapies to control inflammation and prevent organ damage.

.
Alongside medication, lifestyle adjustments play an equally important role. Sun protection is crucial, as ultraviolet exposure can trigger flare-ups in many patients. Doctors also recommend adopting anti-inflammatory habits, including a balanced diet, regular physical activity, adequate sleep and effective stress management. These measures help reduce overall disease activity and improve quality of life.
The bottom line
Lupus is not just a medical condition, it also reflects a deeper, systemic issue in how women’s health concerns are often perceived and addressed. Fatigue, pain and recurring complaints are frequently attributed to stress or hormones, delaying diagnosis in many cases.A key concern is how often women’s pain and recurring symptoms are normalized or minimized, leading to what many patients describe as a long and frustrating journey before receiving a correct diagnosis.As many clinicians point out, improving outcomes in lupus is not only about advancing treatments, but also about changing the way women’s health concerns are acknowledged from the very beginning.









Leave a Reply